Hundreds of laboratory technicians, nurses, and other health workers developed cutting-edge skills.
Pneumonia is a leading cause of death in children worldwide and we need updated evidence about its current causes
Pneumonia sickens about 150 million children every year,1 Nair H, Simoes EAF, Rudan I, et al. Global and regional burden of hospital admissions for severe acute lower respiratory infections in young children in 2010: A systematic analysis. Lancet. 2013;381(9875):1380-1390. doi:10.1016/S0140-6736(12)61901-1 and hospitalizes at least 11 million.
About 900,000 children die of pneumonia annually—more children than HIV, TB, Zika, Ebola, and malaria combined.2 Liu L, Oza S, Hogan D, et al. Global, regional, and national causes of under-5 mortality in 2000-15: an updated systematic analysis with implications for the Sustainable Development Goals. Lancet 2016; 388: 3027–35.
The main causes of pneumonia today are not the same as they were in past decades, in part due to successful vaccines. H. influenzae and pneumococcal disease used to be the top causes of pneumonia but widespread use of effective vaccines to prevent these diseases is now common. We need updated evidence to understand which bacteria, viruses, and other germs are now causing the majority of severe pneumonia in children.
Because new vaccines take years to develop, today’s pneumonia research is necessary so children of the future can have an even greater opportunity to be healthy and thrive.
To collect this evidence, we conducted the Pneumonia Etiology Research for Child Health (PERCH) Study in settings representative of where severe childhood pneumonia is common.
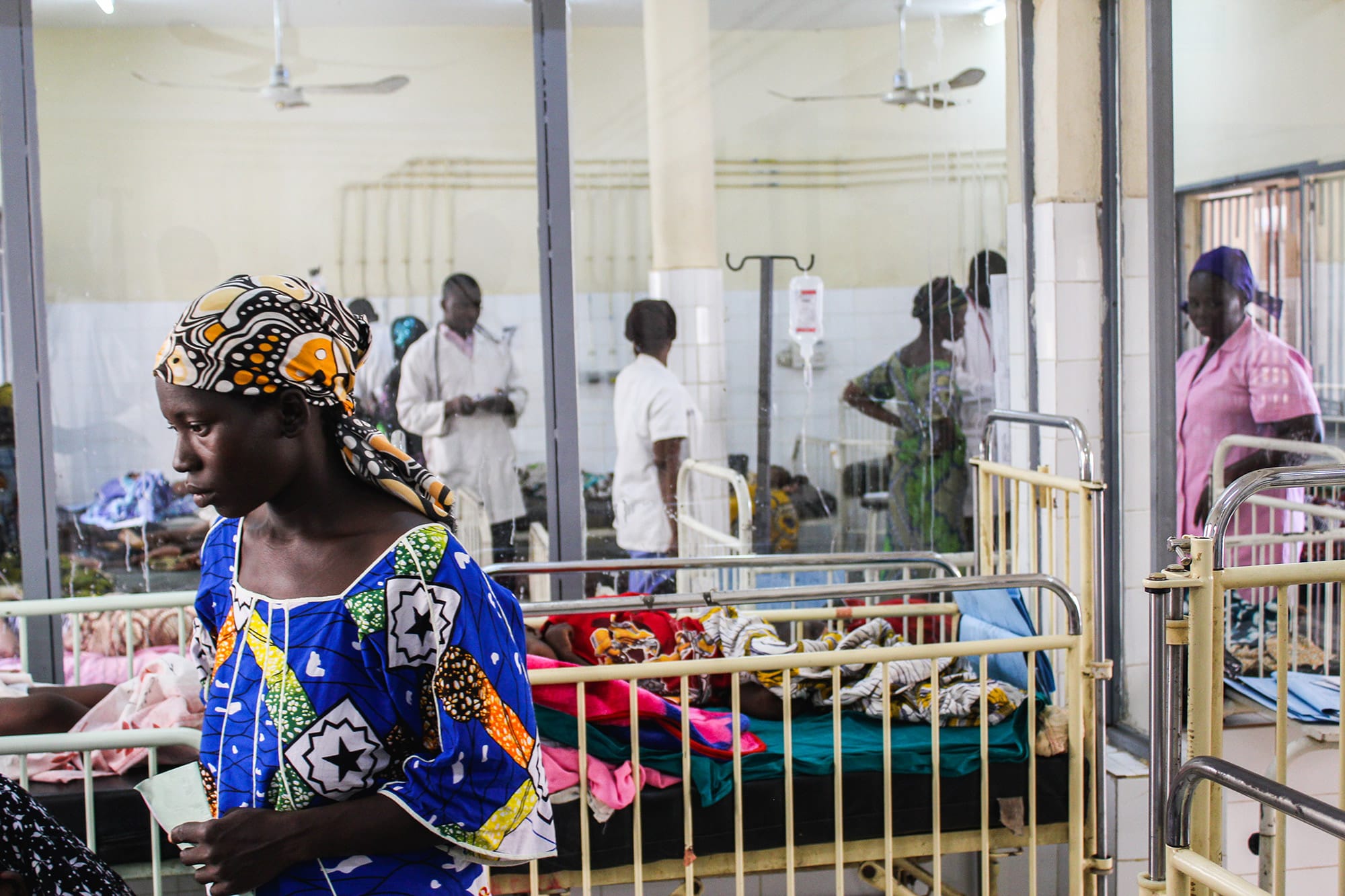


Causes of childhood pneumonia in PERCH
Over the course of two years in 7 countries, the PERCH study team enrolled and tested children hospitalized with pneumonia for the presence of over 30 viruses, bacteria and fungi.
Viruses caused most of the severe pneumonia cases (61%), and respiratory syncytial virus (RSV) was the leading pathogen (31%) at all sites.
Explore 10 of the top causes of severe pneumonia:
10 pathogens caused the vast majority (about 8 in 10 cases): RSV , RSV is a virus that can cause upper and lower respiratory tract illness. rhinovirus , Rhinovirus is the predominant cause of the “common cold.” human metapneumovirus (hMPV) , hMPV is a virus that can cause upper and lower respiratory tract illness. parainfluenza , Parainfluenza is a group of viruses that cause upper and lower respiratory tract illness and are unrelated to influenza (aka “the flu”). pneumococcus , Pneumococcus is a bacterium often found in the nose. It can cause serious illness besides pneumonia like meningitis, blood infections, and ear infections. Haemophilus influenzae , H. influenzae is a bacterium often found in the nose. It can cause serious illness besides pneumonia like meningitis, blood infections, and ear infections. tuberculosis (TB) , TB is a bacterium that mainly infects the lungs. Staphylococcus aureus (Staph) , Staph is a bacterium that is often found on skin and in the nose. Besides pneumonia, it can infect blood, skin, and soft tissue. influenza Influenza, aka “the flu,” is a group of viruses that can cause mild to severe respiratory illness. and Pneumocystis jirovecii . P. jirovecii is a yeast-like fungus that causes pneumonia.
- All ages and cases
- Below age 1
- Above age 1
- Severe cases
- Very severe cases
- The Gambia
- Mali
- Kenya
- Zambia
- South Africa
- Bangladesh
- Thailand
Average in all 7 countries, by:
Average of all ages and severities, in:
RSV is a virus that can cause upper and lower respiratory tract illness. Rhinovirus is the predominant cause of the “common cold.” hMPV is a virus that can cause upper and lower respiratory tract illness. Parainfluenza is a group of viruses that cause upper and lower respiratory tract illness and are unrelated to influenza (aka “the flu”). Pneumococcus is a bacterium often found in the nose. It can cause serious illness besides pneumonia like meningitis, blood infections, and ear infections. H. influenzae is a bacterium often found in the nose. It can cause serious illness besides pneumonia like meningitis, blood infections, and ear infections. TB is a bacterium that mainly infects the lungs. Staph is a bacterium that is often found on skin and in the nose. Besides pneumonia, it can infect blood, skin, and soft tissue. Influenza, aka “the flu,” is a group of viruses that can cause mild to severe respiratory illness. P. jirovecii is a yeast-like fungus that causes pneumonia.
The PERCH study was the largest, most comprehensive pneumonia etiology study conducted in over three decades
Clinicians, governments, donors, and vaccine developers need new evidence on causes of pneumonia from countries where child mortality from pneumonia is still far too high in order to guide updates to treatment and prevention strategies.
The PERCH study used rigorously standardized clinical and laboratory methods and a novel data analysis method that allowed PERCH to identify the causes of pneumonia across the population and in each individual study child—this made PERCH different from any other study of pneumonia.
PERCH enrolled 4,232 children between 1 month and 5 years who were hospitalized with severe pneumonia. Researchers also included 5,325 children from the same communities who did not have severe pneumonia. The study was conducted in 7 countries in Africa and Asia, each country with differing characteristics that might influence the causes of pneumonia. H. influenzae type b vaccine was in routine use at all PERCH sites except Thailand, and pneumococcal conjugate vaccines were in routine use in The Gambia, Kenya, Mali and South Africa. See below to learn more about the study population and study sites.
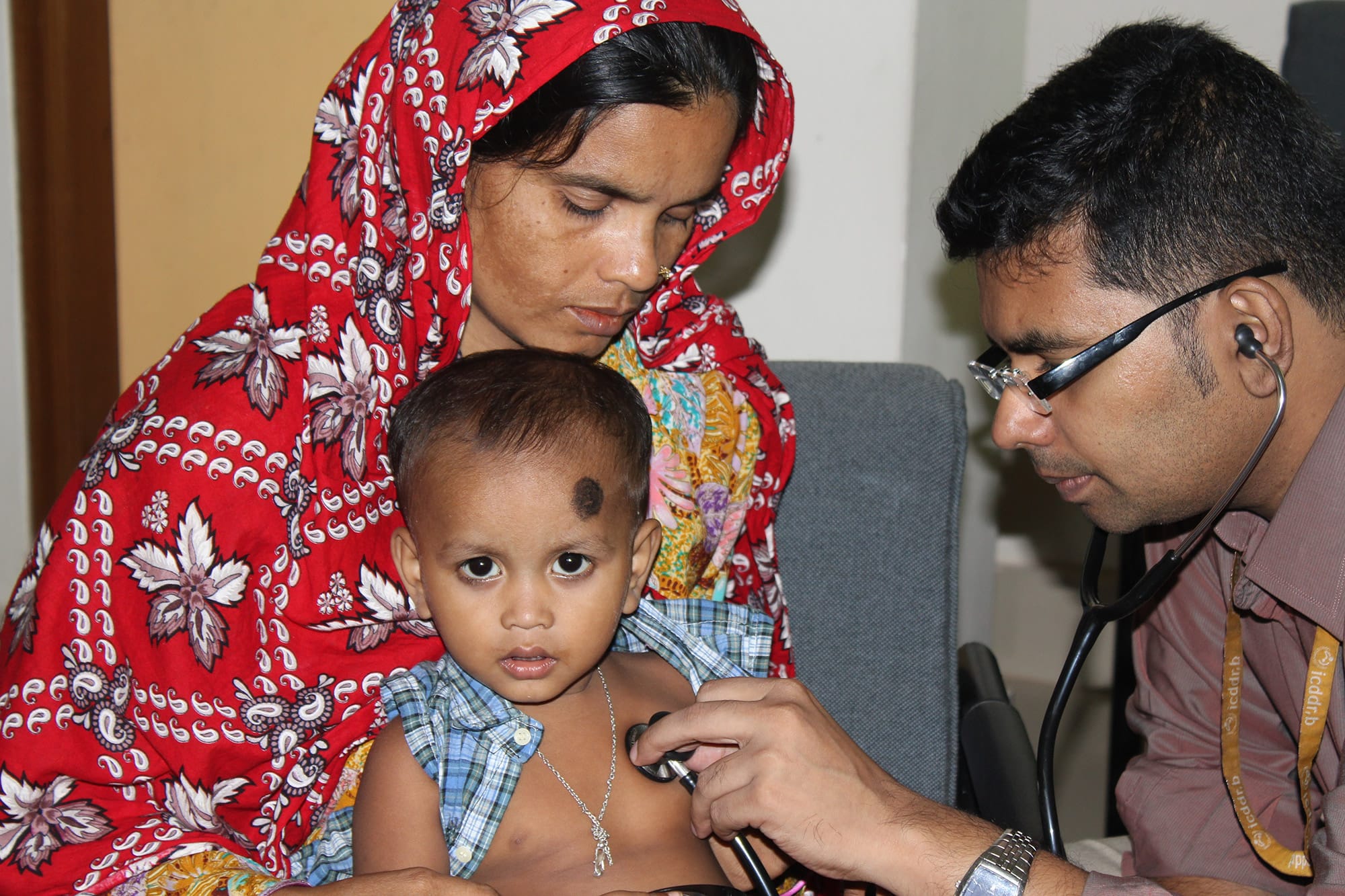

PERCH cases are a subset of all pneumonia cases
Children with pneumonia that resolved before progressing to severe pneumonia, or those who died before they reached the hospital were not included in the PERCH study.
Children enrolled into PERCH were hospitalized with severe or very severe pneumonia, with or without chest x-ray findings.
The proportion of children who died following enrollment varied by site and was up to 1 in 6 children in Zambia and Mali, despite receiving medical care.
Explore the 7 sites:
- {country}, {years}



PERCH’s novel statistical package
It’s very hard to identify the causes of pneumonia in children because it is difficult to access the lung itself. Therefore, scientists and clinicians look for bacteria and viruses in samples from a child’s nose, blood, and other body fluids that may indicate what is infecting the lung.
Yet the utility of these samples alone is limited. Blood culture can only detect bacterial causes, and often yield nothing at all even when the child really does have bacterial pneumonia. Samples from the nose can be misleading since children tend to have many germs in the nose even when they are healthy, none of which may be causing disease in the lungs of children with pneumonia. Therefore, results must factor in findings from multiple samples.
PERCH devised a new way to combine evidence from multiple test results to estimate the causes of pneumonia. The Bayesian Analysis Kit for Etiology Research, or BAKER method, factors in the limitations and strengths of each laboratory test to estimate what’s causing pneumonia in each child. 3, Wu Z, Deloria-Knoll M, Hammitt LL, Zeger SL. Partially latent class models for case-control studies of childhood pneumonia aetiology. J R Stat Soc Ser C Appl Stat 2016; 65: 97–114. 4, Wu Z, Deloria-Knoll M, Zeger S. Nested Partially-Latent Class Models for Dependent Binary Data; Estimating Disease Etiology. Biostatistics 2017; 18: 200–13. 5, Deloria Knoll M, Fu W, Shi Q, et al. Bayesian Estimation of Pneumonia Etiology: Epidemiologic Considerations and Applications to the Pneumonia Etiology Research for Child Health Study. Clin Infect Dis 2017; 64: S213–27. 6 Bayesian Analysis Kit for Etiology Research (BAKER), publicly available at https://github.com/zhenkewu/baker.
BAKER is now “open source” and being used to study other challenging questions like the causes of infection in newborns.
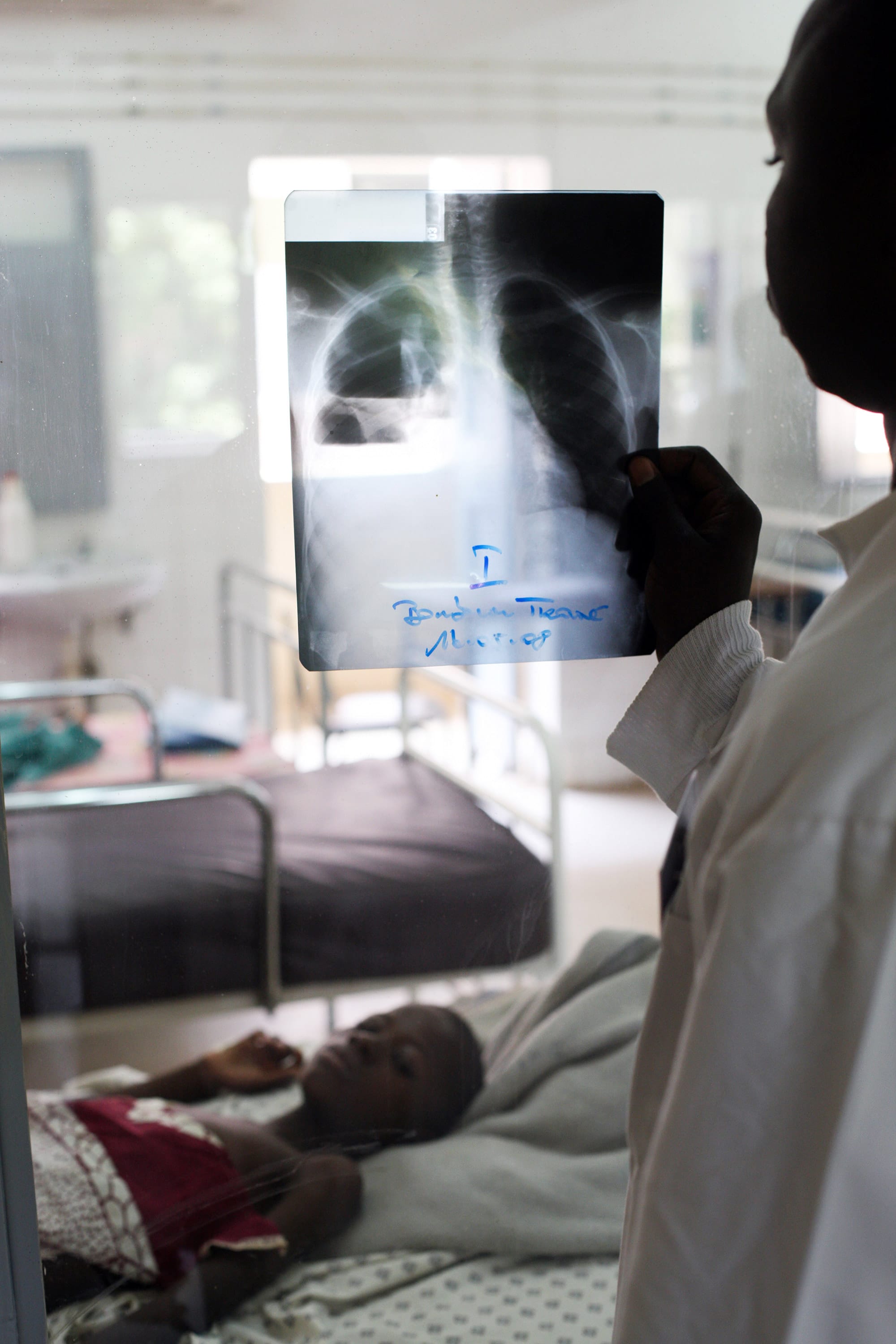
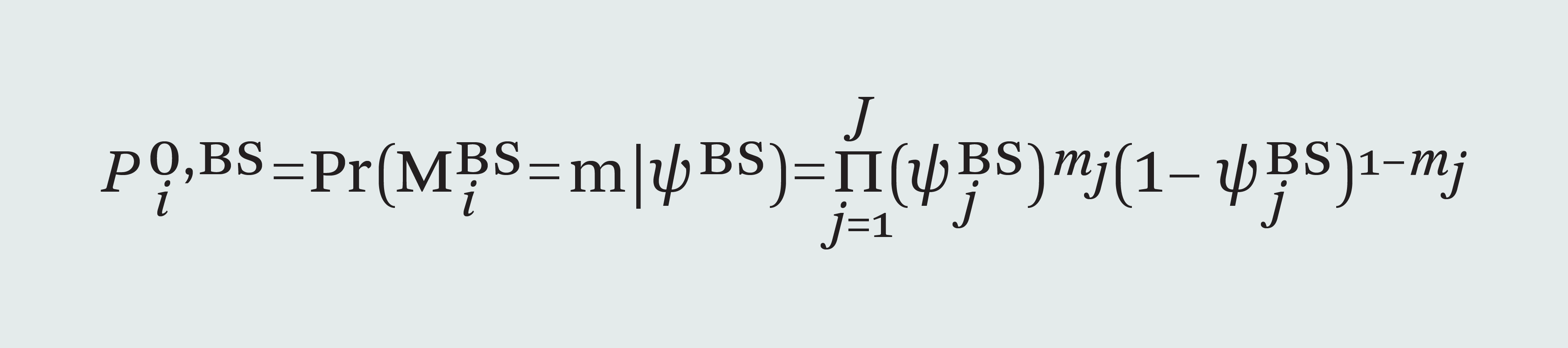
The PERCH study will impact how we prevent, diagnose, and treat pneumonia in the 21st century
By focusing on the leading causes, governments, donors, researchers, and doctors can efficiently reduce child pneumonia illness and death.
Prevent: Scaling up currently-available vaccines and developing new vaccines
PERCH showed that in the settings studied, viruses are more likely to cause severe pneumonia for a child in hospital than are bacteria. We need new vaccines and other products to address this viral burden, especially against the leading causes.
Vaccines and long-acting monoclonal antibodies against RSV are in the late stages of development. New vaccines against influenza, such as a universal flu vaccine that protects against all strains, are now in development. Scientists are also working on vaccines against parainfluenza virus and the Staph bacterium.
Diagnose: Developing new tools to identify the causes of pneumonia
New tools powered by findings from PERCH could help clinicians incorporate multiple test results to more accurately identify what has caused pneumonia for an individual child. Such individualized medicine, in turn, can enable better and smarter treatment of children with severe pneumonia.
Treat: Reducing our reliance on antibiotics
Antibiotics are the standard for treating severe pneumonia.
With PERCH results showing that viral causes predominate, a finding consistent in all settings evaluated by PERCH, and with the development of new tools to help identify the causes of pneumonia, treatment standards may be revised to tailor therapy and reduce antibiotic use.
Reducing the use of antibiotics is one strategy to lower the risk of antimicrobial resistance.

Scientific, Human, and Technological Resources Forged
PERCH was committed to standardizing protocols, methods, testing algorithms, and equipment across all 7 countries.










11 institutions worked together to standardize protocols and train all involved in the research study:
- BALTIMORE, MARYLAND Johns Hopkins Bloomberg School of Public Health, International Vaccine Access Center – central coordinating center
- BASSE, THE GAMBIA Medical Research Council
- KILIFI, KENYA KEMRI-Wellcome Trust Research Programme
- BAMAKO, MALI Center for Vaccine Development, University of Maryland School of Medicine and Centre pour le Developpment des Vaccins (CVD-Mali)
- DHAKA, BANGLADESH icddr,b
- NONTHABURI, THAILAND Thailand Ministry of Public Health – U.S. CDC Collaboration
- JOHANNESBURG, SOUTH AFRICA Medical Research Council: Respiratory and Meningeal Pathogens Research Unit; University of the Witwatersrand
- LUSAKA, ZAMBIA Boston University School of Public Health and University Teaching Hospital
- CHRISTCHURCH, NEW ZEALAND Canterbury Health Laboratories
University of Otago - ROCKVILLE, MARYLAND The Emmes Company
- OXFORD, UNITED KINGDOM Nuffield Department of Clinical Medicine, University of Oxford
Read the full results of PERCH in The Lancet.
Videos and training materials for clinicians on pneumonia diagnosis, measuring clinical signs, and collecting specimens are publicly available.
The study toolkit, including all protocols, data collection forms, and standard operating procedures created in PERCH, are also available to other researchers.
PERCH’s well-cataloged dataset and specimen bank, one of the largest available on childhood pneumonia, are being used by at least 15 external research groups to test, analyze, and pose their own questions. The dataset will soon be publicly available.
The statistical method (BAKER) used to analyze PERCH data is also available for researchers to analyze their data.
Thank you to the families and children who participated in PERCH.
PERCH was supported by a grant from The Bill & Melinda Gates Foundation.
© International Vaccine Access Center 2019. All are free to use facts and representation of findings with attribution.
Suggested Citation:
The PERCH Team. “Visualizing PERCH Results: Etiology of Pneumonia in Children Hospitalized in 7 Countries.” The International Vaccine Access Center: 2019.
www.perchresults.org.
Design by House9
















